Board for Professional Medical Conduct - 2001 Annual Report
Office of Professional Medical ConductNew York State Department of Health
433 River Street, Suite 1000
Troy, NY 12180-2299
- Main Number: 518-402-0836
- Complaints/Inquiries: 1-800-663-6114
- E-mail: opmc@health.state.ny.us
- Web Address: www.health.state.ny.us/nysdoh/opmc/main.htm
George E. Pataki, Governor
Antonia C. Novello, M.D., M.P.H., Dr. P.H., Commissioner of Health
Dennis J. Graziano, Director - Office of Professional Medical Conduct
William P. Dillon, M.D., Chair - Board for Professional Medical Conduct
Michael Gonzalez, R.P.A., Vice Chair - Board for Professional Medical Conduct
Ansel R. Marks, M.D., J.D., Executive Secretary - Board for Professional Medical Conduct
General Program Information
Board for Professional Medical Conduct
The Board for Professional Medical Conduct was created by the New York State Legislature in 1976 and serves as a key resource in the state's disciplinary oversight of physicians and physician assistants.
Public Health Law, Section 230(14) states:
The board shall prepare an annual report for the legislature, the governor and other executive offices, the medical profession, medical professional societies, consumer agencies and other interested persons.
Prior to 1976, the New York State Education Department was responsible for the licensing and disciplining of physicians and physician assistants. In 1976, the state Legislature split the licensing and disciplinary processes between the departments of Education and Health. The board became responsible for investigating complaints, conducting hearings and recommending disciplinary actions to the State Education Department. The State Education Department and the Board of Regents, the department's governing body, were responsible for determining final actions in all physician discipline cases.
In 1991, the physician disciplinary process was again modified by the state Legislature. The Board of Regents and State Education Department were entirely removed from the physician discipline process. The State Education Department retained licensing authority, while the Department of Health assumed disciplinary authority, including the revocation of licenses, for physicians, physician assistants and specialist assistants. The Board for Professional Medical Conduct was granted sole responsibility for determining final administrative actions in all physician, physician assistant and special assistant discipline cases. All other health care professionals (e.g., nurses, dentists, podiatrists, etc.) are licensed and disciplined by the State Education Department.
The board serves as a key component in the state's disciplinary process. The board's objective has been to ensure that the physician disciplinary structure is qualitatively sound and that it is correctly perceived as fair and effective by both physicians and the public. Physician members are appointed by the Commissioner of Health with recommendations for membership received largely from medical and professional societies. The Commissioner of Health, with approval of the governor, appoints lay members of the board. By law, the Board of Regents may appoint 20 percent of the board's membership.
In disciplinary matters, board members serve on committees of three, two physicians and one non-physician, who are appointed by the board chair. Disciplinary committees include investigation, hearing and license restoration. The Administrative Review Board (ARB) is a standing committee consisting of three physicians and two lay members. Board members also serve on a variety of committees that address procedural and emerging policy issues.
The roles of the board and OPMC are delineated in Public Health Law Section 230. The definitions of misconduct are found in Sections 6530 and 6531 of the Education Law.
Office of Professional Medical Conduct
OPMC provides staff to carry out the objectives of the board. OPMC's mission is to protect the public through the investigation of professional misconduct issues involving physicians and physician assistants. Through its investigative and monitoring activities, OPMC strives to deter medical misconduct and promote and preserve standards of medical practice.
The Office:
- Investigates all complaints and, with assistance of counsel, prosecutes physicians formally charged with misconduct.
- Monitors physicians whose licenses have been restored following a temporary surrender due to incapacity by drugs, alcohol or mental impairment.
- Oversees the contract with the Medical Society of the State of New York's Committee for Physicians' Health (CPH) — a non-disciplinary program to identify, refer to treatment and monitor impaired physicians.
- Monitors physicians and physician assistants placed on probation.
- Supports the activities of the 159-member Board for Professional Medical Conduct, including managing the appointment process, training, assisting with committee work and policy development, recruitment of medical experts, and coordinating the canvass procedures for approximately 150 hearing panels annually.
Overview of New York's Medical Conduct Process
OPMC received 6,983 complaints in 2001. It is required by law to investigate every complaint it receives. Many complaints involve issues over which OPMC has no jurisdiction or authority, such as billing disputes or physician rudeness. In these instances, a physician is not aware of the complaint because they are closed administratively. In other cases, a complaint is investigated but insufficient evidence is found to support charges of misconduct, and the investigation is concluded.
When someone does file a complaint with OPMC that appears to involve possible misconduct, the physician will be notified either by letter or through a phone call. Generally, unless specifically stated otherwise, a letter requesting patient records is an indicator that a complaint has been filed against a physician and an investigation is underway. An investigator may call and say there is a complaint and ask for records or to discuss the matter.
State Public Health Law requires OPMC to keep confidential the names of any individuals who file complaints. The source of a complaint may not be the patient whose medical records are requested, but rather a friend, relative or health care worker. Sometimes patient medical records are requested because a health facility has reported to OPMC, as required by law, that it has taken disciplinary action against a physician.
While the law protects the identity of the complainant, it also preserves a physician's right to be heard. State Public Health Law requires that a physician be given the opportunity to be interviewed by OPMC staff to provide an explanation of the issues under investigation if the matter is going to be referred to the board. This interview may be conducted in person or over the telephone, and the physician may have an attorney present.
In many cases, even if the matter does not result in a referral to the board, the physician is contacted to respond to the issues in the complaint. Cases are not referred to the board when there is insufficient evidence to proceed or the issues are out of its jurisdiction. Physicians contacted in such cases are advised by letter that the matter is closed.
When an investigation finds evidence that appears to indicate that misconduct has occurred, the evidence presented to an investigation committee of the board for review. If the investigation committee, consisting of two physicians and a lay member drawn from the board, finds sufficient evidence to support misconduct charges, it is recommended to the director that charges be served and the case will proceed to a hearing.
The committee may recommend to the Commissioner of Health that a physician's practice be summarily suspended because he or she poses an imminent danger to the public health. Committee members can also order non-disciplinary administrative warnings or consultations. If the committee finds there is not sufficient evidence to support charges, the physician receives a closure letter indicating the investigation has concluded.
If the case is voted to a hearing or the Commissioner of Health orders a summary suspension, another three-member panel, including two physicians and a lay member, is drawn from the board. A hearing is much like a trial, although in this case the board panel serves as the jury and may also ask questions. An administrative law judge is present to assist the panel on legal issues. The state's case is presented by a staff attorney and physicians generally also choose to be represented by counsel. At the hearing, evidence is presented and testimony may be given by witnesses for both sides.
Public Health Law requires that hearings start within 60 days of the service of charges or, in cases of summary suspension, the hearing must commence within 10 days of the service of charges. The last hearing day must be held within 120 days of the first hearing day. The hearing panel's decision must be issued within 60 days of the last hearing day. Changes in these time frames can be made by agreement of both sides.
A hearing panel may decide to dismiss some or all of the charges against a physician. If the panel sustains charges, penalties can range from a censure and reprimand to revocation. The panel may also suspend or annul a physician's license, limit his or her practice, require supervision or monitoring of a practice, order retraining, levy a fine or require public service. Revocations, actual suspensions and license annulments are immediately made public and penalties go into effect at once.
Other penalties are not made public until the period for requesting an appeal has passed and, if there is an appeal, disciplinary action is stayed until there is a resolution. Either side may appeal the decision of a hearing panel to the ARB.
Notices of appeal must be filed within 14 days of the service of a hearing committee decision. Both parties have 30 days from the service of the notice of appeal to file briefs and then another seven days to file a response to the briefs. There are no appearances or testimony in the appeals process. During an appeal, revocations, actual suspensions and annulments are not stayed. However, other penalties are stayed until the ARB acts.
The ARB reviews whether or not the determination and penalty of the hearing committee are consistent with the hearing panel's findings and whether the penalty is appropriate. The ARB must issue a written determination within 45 days after the submission of briefs.
The Year in Review
Board Activities
Special Board Committees
The Joint Committee between the Committee for Physicians' Health (CPH) and the Board for Professional Medical Conduct (BPMC) is charged to develop recommendations that will enhance the continued efforts of New York State's impaired physician programs to both protect the public and assist physicians in need. At the February 5, 2001 meeting of the Joint CPH-BPMC Committee of the Impaired Physicians Programs, two subcommittees were appointed and charged with reviewing two specific issues (boundary issues and the restoration process) and making recommendations for the committee's consideration. Each subcommittee consists of four Joint CPH-BPMC Committee members and one staff person from each program.
Physician/Patient Boundary Issues
The Subcommittee on Boundary Issues addressed concerns that physicians may not be fully aware of the issues and consequences surrounding boundary violations. The subcommittee focused on developing educational materials that would address several types of boundary issues, including financial, social and sexual, for physicians. Working with the authors' permission, the subcommittee modified an article entitled "Professional Boundaries in the Physician-Patient Relationship" by Glenn Gabbard, M.D. and Carol Nadelson, M.D. The subcommittee is exploring various routes of circulation among the medical community including the physician license registration process. Release of a brochure is planned for summer 2003.
Enhancing the Restoration Process
Each year about 12 physicians petition the board for approval to return to the active practice of medicine following treatment for their addictions. The restoration process involves a formal proceeding during which a board committee reviews records and hears testimony attesting to the fitness of the physician to practice safety and competently. Although not required, physicians are usually accompanied by legal counsel. Written procedures to help guide physicians and their attorneys through the restoration process are being developed and will be presented to the Joint CPH-BPMC Committee in summer 2003.
The Subcommittee on Enhancing the Physician's License Restoration Process identified the following activities that would enhance the restoration process:
- Preparing written procedures to guide the process
- Identifying additional behavioral health specialists to conduct clinical assessments
- Educating and training BPMC members in the areas of addiction and recovery
- Identifying "milestones" of recovery
The impaired physicians programs currently utilize one of four national centers specializing in the evaluation and treatment of impaired medical professionals in making the determination of impairment. A new assessment program has been identified at the Columbia Presbyterian Medical Center in northern Manhattan. The subcommittee will also assess whether the Columbia Neuropsychiatric Evaluation Service might be a useful resource for our programs.
Three regional BPMC training seminars on the impaired physician were held in New York City and Syracuse and nearly all board members attended. Participant evaluations were highly complimentary of the training and it is expected that an advanced training program will be offered to board members in summer 2003.
The subcommittee will continue to identify those lifestyle behaviors that are supportive of long-term recovery from addiction.
Annual Meeting
The 2001 Biennial Meeting of the Board for Professional Medical Conduct was held in Albany on November 2-4, 2001. One hundred and twenty-eight members, representing over 80 percent of the board, attended the weekend session. This meeting was part of the board's ongoing efforts to provide training on issues pertinent to today's practice of medicine and the disciplinary system.
Specialists working in the forefront of medicine discussed such exciting and pertinent topics as the ethics of the new medicine, including virtual reality medicine, the genome project, organ allocation and medical research.
Training for board members focused on analyzing the elements of a board decision (developing consistency between the finding of facts, discussion and penalty). Sessions also provided updates on Department of Health and OPMC activities regarding physician profiling, fraud and office-based surgery. Special guest speakers included Commissioner of Health Antonia C. Novello, M.D., M.P.H., Dr.P.H. and Chief Judge Judith Kaye of the New York State Court of Appeals.
National Recognition
The Federation of State Medical Boards of the United States (FSMB), at its annual meeting, re-elected Fr. Daniel Morrissey to a three-year term on its board. Charles J. Vacanti, M.D. was elected to the Nominations Committee, a one-year post. Thea Graves Pellman continues to serve on the Editorial Committee. Datta G. Wagle, M.D. was appointed to the Program Committee and Kendrick Sears, M.D. was appointed to the Bylaws Committee.
Program Highlights
- New York placed first in the nation in the total number of serious disciplinary and loss of license actions according to the FSMB.
- Improvements were made to the Department of Health's Web site. A new version of the physician discipline database has been implemented, featuring a direct link from the physician profiling system and an improved search engine. The site now includes information on disciplinary actions taken against physicians dating back to 1990 as well as the text of board determinations and orders. In 2001, the site received nearly two million hits from more than 301,000 visitors, reflecting a 33 percent increase in activity over the previous year.
- The Public Citizen's Health Research Group reported that New York was one of only seven states in the nation to receive an "A" for both the content and user friendliness of its disciplinary action Web site.
- The Public Citizen's Health Research Group ranked New York 14th in the nation, up from 49th in 1991, in the rate of serious disciplinary actions per licensed physician.
- During the last five years, the number of complaints received has increased an average of 6 percent per year. In 2001, OPMC experienced a dramatic rise in the number of complaints. OPMC received a record 6,983 complaints in 2001, representing a 13 percent increase over complaints received in the previous year.
- The average length of time for case prosecution decreased from six months in 1996 to five months in 2001.
- OPMC continued to aggressively prosecute physicians who violate their terms of probation by referring 33 physicians for prosecution and taking 11 disciplinary actions, 10 of which involved loss of license.
- In 2001, investigation committees recommended 155 administrative warnings be administered to physicians and/or physician assistants, 80 of which were done in person. This represents a 28 percent increase in administrative warnings administered to physicians and/or physician assistants.
Investigative Capabilities
- A pilot program was developed and implemented to quickly resolve simple cases without the need for time-consuming and resource-depleting investigations. During the last six months of 2001, 68 cases were resolved to the satisfaction of both parties. Statewide implementation of this system is being evaluated.
- The fees paid to medical experts were increased to ensure the availability of qualified physicians for case review and testimony.
The Corporate Practice of Medicine
During 2001, the board took its first action against business entities that practice medicine. Ten professional corporations (PCs) and one registered limited liability partnership (RLLP) were disciplined for fraudulent practice reasons. All 11 entities had their certificates of incorporation revoked, or in the case of the RLLP, its certification of registration was revoked. Five of the 11 entities were disciplined after hearings and three of those were fined $10,000 each. The remaining six entities were disciplined through consent agreements and orders.
This proactive initiative against business entities is based on the premise that from a public health perspective, it is difficult for unsuspecting patients to discern whether business entities that practice medicine are fraudulently established by physicians and then overseen and operated by non-physicians. Disciplining the business entities has the effect of interrupting, and protecting, the stream of patients that frequent these businesses with the expectation of receiving competent medical care. From a billing fraud perspective, these business entities are the primary generators of medical bills in the health care industry and are the primary repository for proceeds from those bills. Disciplining the business entities has the effect of prohibiting money flow in schemes to defraud. Accordingly, business entities that practice medicine fraudulently or incompetently can be just as harmful to the public health as individual physicians who practice medicine fraudulently or incompetently.
Communication and Outreach
During the past year, technological enhancements were implemented resulting in greater and easier access by the public to information regarding physicians and disciplinary actions.
Final Actions Database
- A new version of the final actions database, replacing three previously used databases, was implemented, featuring a direct link from the physician profiling system. The public can view the latest disciplinary action without accessing multiple Web sites and without having to enter a second query.
- An improved search engine that permits searching the database as opposed to searching text files was deployed. This allows tailoring the search to ranges of values, e.g. disciplinary actions updated within the last week. It also precludes false matches caused by the text-based search engine. There are several pre-defined searches contained in the new database, including type (MD, DO or RPA), physician name, license and effective date of the action.
- The new database allows a person to subscribe and be notified that there has been a change to the disciplinary action information.
Office of Professional Medical Conduct Summary Statistics
| Action | Year | ||||
|---|---|---|---|---|---|
| 1997 | 1998 | 1999 | 2000 | 2001 | |
| Complaints Received | 5782 | 6440 | 6690 | 6106 | 6983 |
| Investigations Completed | 6453 | 6359 | 6732 | 5939 | 6854 |
| Licensees Referred for Charges | 320 | 354 | 384 | 388 | 367 |
| Administrative Warnings/Consultations | 126 | 103 | 96 | 121 | 155 |
| Summary Suspensions* | 12 | 32 | 23 | 43 | 23 |
| DISCIPLINARY ACTIONS | YEAR | ||||
|---|---|---|---|---|---|
| 1997 | 1998 | 1999 | 2000 | 2001 | |
| Surrender | 93 | 100 | 100 | 97 | 97 |
| Revocation | 81 | 59 | 61 | 47 | 33 |
| Suspension | 92 | 90 | 93 | 105 | 101 |
| Censure and Reprimand/Probation | 33 | 29 | 28 | 34 | 32 |
| Censure and Reprimand/Other | 37 | 34 | 39 | 64 | 44 |
| Dismiss | 6 | 7 | 8 | 10 | 18 |
| SUBTOTAL | 342 | 319 | 329 | 357 | 325 |
| Temporary/Permanent Surrenders | 23 | 28 | 27 | 25 | 18 |
| Monitoring Agreements | 6 | 22 | 24 | 29 | 25 |
| TOTAL ACTIONS | 371 | 369 | 380 | 411 | 368 |
*In 1996, Public Health Law 230 was amended to permit a summary suspension when a licensee has pleaded or been found guilty or convicted of committing an act constituting a felony under New York State Law or federal law, or the law of another jurisdiction which, if committed within this state, would have constituted a felony under New York State law, or when the duly authorized professional agency of another jurisdiction has made a finding substantially equivalent to a finding that the practice of medicine by the licensee in that jurisdiction constitutes an imminent danger to the health of its people....
Disciplinary Actions by the Board for Professional Medical Conduct 2001
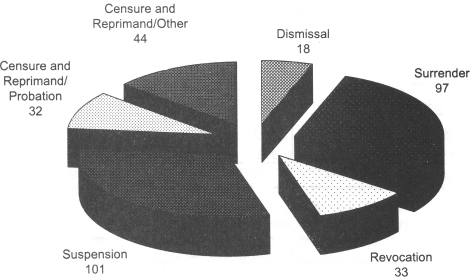
| Disciplinary Action | Total |
|---|---|
| Censure and Reprimand/Other | 44 |
| Censure and Reprimand/Probation | 32 |
| Dismissal | 18 |
| Revocation | 33 |
| Surrender | 97 |
| Suspension | 101 |
Office of Professional Medical Conduct Source of Complaints 2001
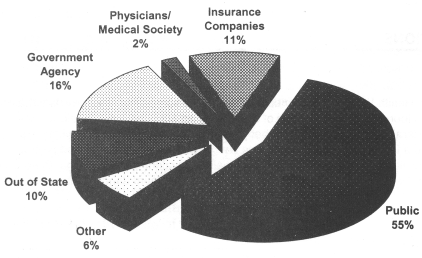
| Source of Complaint | Percentage |
|---|---|
| Government Agency | 16% |
| Insurance Companies | 11% |
| Other | 6% |
| Out of State | 10% |
| Physicians/Medical Society | 2% |
| Public | 55% |