DOH Medicaid Update March 2005 Vol. 20, No. 4
Office of Medicaid Management
DOH Medicaid Update
March 2005 Vol.20, No. 4
State of New York
George E. Pataki, Governor
Department of Health
Antonia C. Novello, M.D., M.P.H., Dr. P.H.
Commissioner
Medicaid Update
is a monthly publication of the
New York State Department of Health,
Office of Medicaid Management,
14th Floor, Room 1466,
Corning Tower, Albany,
New York 12237
Table of Contents
How and Where Can I Access the List of Medicaid Reimbursable Drugs
Ask The Pharmacist
Notice to Medicaid Clients Concerning Drug Coverage
A Tip on Prior Authorization of Pharmacy Items
Expansion of Managed Care Special Needs Plans Service Areas
Patient Educational Tools: New Dietary Guidelines for Americans 2005
Congestive Heart Failure in New York's Medicaid Population
Attention Providers of Personal Care; Consumer Directed Personal Assistance Programs;
Personal Emergency Response Services; Assisted Living Programs; Limited Licensed Home Care Service Agencies
Managed Care Enrollee Pharmacy Co-Payment Changes
Provider Manuals Go Online
Index of 2004 Medicaid Update Articles
eMedny Update
All Providers
eMedNY Transition Plan Now Available
Return to Table of Contents
The implementation of eMedNY Phase II is imminent. While the Department and Computer Sciences Corporation (CSC) have worked to make your transition to eMedNY as seamless as possible, the new system will require some changes in the manner in which providers interact with the New York State Medicaid program. The changes you need to implement may differ based on whether you bill electronically or by paper claim forms. These changes are outlined in the eMedNY Phase II HIPAA Transaction Information, which is accessible at the website www.nyhipaadesk.com, (click on the "News and Resource" tab and look below "Important Notice").
Understanding that some providers may have difficulty in making their required changes for eMedNY Phase II by the March 24 implementation date, the Department is offering a short-term Transition Plan to assist these providers in their migration. This Transition Plan will be available for only a three-month period, ending June 20, 2005. To utilize Transition Plan processing, providers will be required to submit an Application for Transition Processing signed by the CEO or highest ranking officer of the organization. A copy of the Application was mailed to all providers last month with the letter originally announcing the Transition Plan; to obtain another copy, call CSC Provider Services at (800) 522-5518 or (518) 447-9860.
This offer will not be available to providers that have not made their conversion to HIPAA. Non-compliant transactions will be accepted until March 21, 2005. Non-compliant claims filed after that date will be rejected from processing.
Providers should not wait until the June 20 deadline to implement their Phase II changes. Claims being submitted in a pre-Phase II format will require additional processing by the Department's fiscal agent (CSC). After May 9, 2005, this additional processing will result in a two-week delay in processing.
The transition plan for electronic submissions includes the following provisions:
- Providers that have not completed their eMedNY Phase II conversion will still be able to send pre-Phase II HIPAA compliant 837 claims to Medicaid during the transition period.
- Hospitals that bill for ordered ambulatory services may continue to submit their claims in the pre-Phase II Institutional (837I) transaction format after March 24, 2005 and until the post-Phase II transaction format is available.
- Providers will be able to continue to use their existing communication methods (MMIS Electronic Gateway or magnetic media) during the three-month contingency plan period while they complete their migration to eMedNY Phase II methods.
- Providers will be able to perform end-to-end testing by submitting both pre-Phase II compliant claims to the current Legacy MMIS location and eMedNY Phase II HIPAA-compliant claims to eMedNY at the same time, and comparing results; correctly formatted claims will be denied by the duplicate claim edits.
The transition plan for paper claims includes the following:
- Providers who will not be ready to submit the new Phase II paper claim forms can continue to use the old ones up through May 31, 2005. However, after May 31, 2005 only new Phase II paper claim forms will be accepted for processing.
This transition plan will not include:
- Support for non-HIPAA electronic transactions. Providers who are not HIPAA-compliant must complete their migration to HIPAA prior to March 21, 2005.
- Support for pre-Phase II HIPAA Eligibility and Service Authorization transactions. Providers must make minor changes to convert their Eligibility and Service Authorization requests to HIPAA Phase II compliance.
- Electronic Remittances (835 and 820 formats) will be formatted using eMedNY Phase II requirements. They will be delivered via eMedNY eXchange or file transfer protocol (FTP). For more information about eMedNY eXchange or FTP, please visit www.emedny.org. Providers will still have the option of selecting paper remittances.
Prior Authorizations and Utilization Threshold Override Applications modified as follows as eMedNY is implemented:
- New Phase II paper forms for Prior Authorizations and Utilization Threshold Override Applications (TOAs), will be required beginning March 21, 2005.
- New Phase II paper forms for Prior Approval types [01-Physician, 03-Dental, 04-Nursing Home/Bed Reservation, 06-DME, 07-Eye Care, 08-Hearing Aid, and 10-Private Duty Nursing], are required beginning on March 14, 2005.
The Department is committed to working with you to achieve a successful implementation of eMedNY Phase II. If you have any questions or need technical clarification, please contact the CSC Provider Services at 800-522-5518 or (518) 447-9860.
If you have any questions or need technical clarification, please contact the CSC Provider Services at (800) 522-5518 or (518) 447-9860.
Attention Pharmacists
HOW AND WHERE CAN I ACCESS
THE LIST OF MEDICAID REIMBURSABLE DRUGS?
Return to Table of Contents

The list of Medicaid reimbursable drugs is available on the internet by accessing the following website:
http://www.emedny.org/info/formfile.html
Once in the website, the list of Medicaid reimbursable drugs can be accessed in one of three ways:
- View/Download PDF file
This file gives you the list of the Medicaid reimbursable drugs in alphabetical order for each of the following: Rx (legend drugs) first, followed by federally scheduled (2-5) controlled drugs, over-the-counter (OTC) products and supplies. - View/Download Excel Spreadsheet
This file can be downloaded and manipulated if desired. This file includes the same information as the PDF file on Rx (legend drugs) and federally controlled drugs. It does not include any headings or any OTC or supply product information. Please refer to PDF file for that information. - There is also a "Find Formulary File Information" function that can be used to search the file. Please refer to the Search tips listed on the website. For example, if you want the list of all NDCs for a drug:
- in the field space, click on description
- in value space, put in name of drug
- sort by NDC
Ordering Providers:
This information is updated once a month. Therefore, it does not reflect any changes made to the file within the month.
Pharmacy Providers:
If you do not have internet access and want to check the availability of a NDC, you can submit a claim and reverse it if necessary.
If you have any questions, please contact the Pharmacy Policy and Operations staff at (518) 486-3209.

PROVIDER SERVICES
Return to Table of Contents
Comments and Suggestions Regarding This Publication?
Please contact the editor, Timothy Perry-Coon, at:
MedicaidUpdate@health.state.ny.us or
via telephone at (518) 474-9219 with your concerns.

Ask the Pharmacist....
Return to Table of Contents
- Q: Over the past year I have been in situations where Medicaid recipients of male gender request to have a prescription for estrogen filled. Claims are rejecting with a message "Drug not valid due to recipient sex", where in the past, they did not. Please clarify this coverage issue for my customers and staff.
- A: Recently, Medicaid's pharmacy claims processing system was upgraded to validate gender specific drug requirements prior to payment. Claims for pharmaceuticals that are typically indicated for females, like estrogen, will deny at the pharmacy if the patient's gender is listed as "male" on the eligibility file. Section 505.2 of NYCRR 18 states: "Payment is not available for care, services, drugs, or supplies rendered for the purpose of gender reassignment (also known as transsexual surgery) or any care, services, drugs, or supplies intended to promote such treatment."
- Q: Periodically we receive a letter referencing FUL. What is FUL and are these communications for my store's information, or is any action required?
- A: FUL stands for Federal Upper Limit. The FUL program caps Medicaid payments for brand name and generic drugs that are therapeutically equivalent and meet certain criteria. As a result, the FUL program, which achieves savings by taking advantage of current market prices, helps to reduce pharmacy costs for both the states and the federal government.
The Centers for Medicare and Medicaid Services (CMS) notifies all State agencies whenever there are price increases, decreases and labeler participation changes. New York State passes on this information regarding any changes that may have occurred. This is for informational purposes only and no action is required by your store.
- A: FUL stands for Federal Upper Limit. The FUL program caps Medicaid payments for brand name and generic drugs that are therapeutically equivalent and meet certain criteria. As a result, the FUL program, which achieves savings by taking advantage of current market prices, helps to reduce pharmacy costs for both the states and the federal government.
- Q: Which drugs are covered for weight loss?
- A: The New York State Medicaid program does not provide coverage for any drug indicated for the purpose of weight reduction. Section 1927(d) of the federal Social Security Act provides that drugs used for the purpose of weight loss or gain are excludable from Medicaid coverage. On the other side of this page is a notice you may wish to display in your store explaining that Medicaid does not cover all drugs.
Pharmacists & Prescribers! Do you have questions concerning Drug Coverage?
A review of our telephone statistics indicates a large percentage of incoming calls are inquiries concerning whether a drug or a particular NDC is covered by New York State Medicaid. This information can be directly accessed by viewing the list of Medicaid reimbursable drugs at: http://www.eMedNY.org/info/formfile.html. Using this website will save you time and our Pharmacy Policy staff will be free to answer policy-specific questions.
If you have any questions you would like to see published in "Ask the Pharmacist" please e-mail the Pharmacy Policy and Operations mailbox at ppno@health.state.ny.us and indicate in the subject field of your mail: Ask the Pharmacist.


NEW YORK STATE DEPARTMENT OF HEALTH
ALBANY, NEW YORK 12237
ANTONIA C. NOVELLO, M.D., M.P.H., Dr. P.H.
COMMISSIONER
NOTICE TO
MEDICAID CLIENTS
CONCERNING DRUG COVERAGE
Return to Table of Contents
Medicaid is a federal and State funded health insurance program that helps many people who can't afford medical care to pay for some or all of their medical bills.

Items which may be excluded from coverage:
- Agents used for weight loss or weight gain
- Agents used to promote fertility
- Agents used for cosmetic purposes or hair growth
Medicaid covers an extensive number of medically necessary drugs. However, not all drugs are covered.
Check with your pharmacist if you are not sure if a drug you were prescribed is covered by Medicaid.
Attention Prescribers
and
Pharmacists
A Tip on Prior Authorization of Pharmacy Items
Use of the Voice Interactive Phone System
Return to Table of Contents

The Pharmacy Policy and Operations staff are aware that some of you may experience difficulty when entering the recipient identification number to the Voice Interactive Phone System (VIPS). The following tip should be helpful when accessing the VIPS.
Entering a recipient identification number is a two step process:
- Entering the Recipient Identification Number
The VIPS instructs you to record the identification number into your telephone's key pad by selecting the keys that correspond to the letters and numbers of the identification card.
For example, if the identification number is AB12345Z , you will be recording numbers 2 2 1 2 3 4 5 9 via your key pad. - Verification of the Recipient Identification Number
The VIPS will then verify the first two numbers you selected and ask you to identify the first two alphabetic characters of the identification number (AB 12345Z).
a) VIPS will announce, "The first key you pressed was a 2. For the letter A, press 1". You should select the 1 to verify the letter A of the identification number.
b) The VIPS continues: "The second key you pressed was a 2. For the letter A, press 1. B press 2." Now you should select the 2 to verify the letter B of the identification number.
The VIPS now skips over the next five numerals to verify the last alphabetic character of the identification number, and continues: "The eighth key you pressed was a 9. For the letter W press 1. X press 2. Y press 3. Z press 4". Finally, you should select the 4 to verify the letter Z of the identification number.
Please remember to listen carefully to the voice prompts.
For questions regarding this article, please contact the Pharmacy Policy and Operations staff at: (518) 486-3209
EXPANSION OF MANAGED CARE SPECIAL NEEDS PLANS SERVICE AREAS
Return to Table of Contents
Medicaid recipients in New York City have the option to enroll in the following service areas for five Special Needs Managed Care Plans. Providers should make note of these codes in their Provider Manual under the heading "Recipient Other Insurance Codes".
| Medicaid Provider Name | MEVS code on Verifone | 10 characters in eMedNY window | Service Area |
| FidelisCare Healthier Life SN | OF | FIDELIS SN | Bronx, Brooklyn, SI, Manhattan, Queens |
| Healthfirst PHSP Inc SN | OH | HLTHFST SN | Bronx, Brooklyn, Manhattan, Queens |
| NYPS Select Health SN | OG | NYPSSEL SN | Bronx, Brooklyn, Manhattan |
| VidaCare Inc. SN | OD | VIDACARE SN | Bronx, Brooklyn, Manhattan |
| MetroPlus Partnership in Care Plan SN | OM | METROPLUS SN | Bronx, Brooklyn, Queens, Manhattan |
* Please contact the health plans as follows for Special Needs Plan (SNP) benefit package information.
| NYPS SelectHealth SN Provider Relations (866) 469-7774 | VidaCare Inc SN Provider Inquiry (800) 556-0674 | Fidelis Care Healthier Life SN
Provider Relations Call Center (888) FIDELIS (888) 343-3547 |
| MetroPlus Partnership in Care Plan SN Provider Relations Call Center (212) 908-8883 | Healthfirst PHSP SN Provider Relations (888) 801-1660 |
Enrollees can call the New York Medicaid CHOICE Helpline at (800) 505-5678 to find out more about Special Needs Plans.
Additional Special Needs Plan billing information and exceptions for mental health and chemical dependency providers may be found in the August 2004 Medicaid update at http://www.health.state.ny.us/health_care/medicaid/program/main.htm
Questions regarding this article can be directed to the Department of Health at (518) 486-1383.

PATIENT EDUCATIONAL TOOLS
Return to Table of Contents
This month's patient educational tools feature
"New Dietary Guidelines for Americans 2005"
The Medicaid program encourages practitioners to copy and distribute the following information to their patients and to share it with their colleagues.
__________________________________________________________________________

New Dietary Guidelines for Americans 2005
Finding Your Way to a Healthier You:
Health and Human Services Secretary Tommy G. Thompson and Agriculture Secretary Ann M. Veneman announced the release of the Dietary Guidelines for Americans 2005 , the federal government's science-based advice to promote health and reduce risk of chronic diseases through nutrition and physical activity.
Almost two-thirds of Americans are overweight or obese, and more than half get too little physical activity. The sixth edition of Dietary Guidelines for Americans places stronger emphasis on reducing calorie consumption and increasing physical activity. This joint project of the Departments of Health and Human Services and Agriculture is the latest of the five-year reviews required by federal law.
The new guideline highlights how to:
- Make smart choices from every food group.
- Find your balance between food and physical activity.
- Get the most nutrition out of your calories.
A healthy eating plan is one that:
- Emphasizes fruits, vegetables, whole grains, and fat-free or low-fat milk and milk products.
- Includes lean meats, poultry, fish, beans, eggs, and nuts.
- Is low in saturated fats, trans fats, cholesterol, salt (sodium), and added sugars.
Mix up your choices within each food group:
- Focus on fruits. Eat a variety of fruits- whether fresh, frozen, canned, or dried. For a 2,000 calorie diet, you will need 2 cups of fruit each day (for example, 1 small banana, 1 large orange and 1/4 cup of dried apricots or peaches).
- Vary your veggies. Eat more dark green veggies such as broccoli, kale and other dark leafy greens; orange veggies, such as carrots, sweet potatoes, pumpkin, and winter squash; and beans and peas, such as pinto beans, kidney beans, black beans, garbanzo beans, split peas, and lentils.
- Get your calcium-rich foods. Get 3 cups of low-fat or fat-free milk or an equivalent amount of low-fat yogurt and/or low-fat cheese (1 1/2 ounces of cheese equals 1 cup of milk) every day. For kids aged 2-8, it's 2 cups of milk. If you don't or can't consume milk, choose lactose-free milk products and/or calcium-fortified foods and beverages.
- Make half your grains whole. Eat at least 3 ounces of whole-grain cereals, breads, crackers, rice, or pasta every day. One ounce is about 1 slice of bread, 1 cup of breakfast cereal, or 1/2 cup of cooked rice or pasta. Look to see that grains such as wheat, rice oats, or corn are referred to as "whole" in the list of ingredients.
- Go lean with protein. Choose lean meats and poultry. Bake it, broil it, or grill it. Vary your protein choices with more fish, beans, peas, nuts, and seeds.
- Know the limits on fats, salt and sugars. Read the Nutrition Facts label on foods. Look for foods low in saturated fats and trans fats. Choose and prepare foods and beverages with little salt (sodium) and/or added sugars (caloric sweeteners).
Find your balance between food and physical activity. * Becoming a healthier you isn't just about eating healthy - it's also about physical activity. Regular physical activity is important for your overall health and fitness. It also helps you control body weight by balancing the calories you take in as food with the calories you expend (burn) each day.
- Be physically active for at least 30 minutes most days of the week.
- Increasing the intensity or the amount of time that you are physically active can have even greater health benefits and may be needed to control body weight. About 60 minutes a day may be needed to prevent weight gain.
- Children and teenagers should be physically active for 60 minutes every day, or most every day.
- If you have any health issues or concerns, you should talk to your doctor before starting an exercise program.
Get the most nutrition out of your calories. There are a right number of calories for you to eat each day. This number depends on your age, activity level, and whether you're trying to gain, maintain, or lose weight. 2,000 calories is the value used as a general reference on the food label. You can calculate your number at www.healthierus.gov/dietaryguidelines or ask your doctor.
Play it safe with food. Know how to prepare, handle, and store food safely to keep you and your family safe.
- Clean hands, food-contact surfaces, fruits, and vegetables. To avoid spreading bacteria to other foods, meat and poultry should not be washed or rinsed.
- Separate raw, cooked, and ready-to-eat foods while shopping, preparing or storing foods.
- Cook meat, poultry, and fish to safe internal temperatures to kill microorganisms.
- Chill perishable foods promptly and thaw foods properly.
About alcohol. If you choose to drink alcohol, do so in moderation. Moderate drinking means up to 1 drink a day for women and up to 2 drinks for men. Twelve ounces of regular beer, 5 ounces of wine, or 1 1/2 ounces of 80-proof distilled spirits count as a drink for purposes of explaining moderation. Remember that alcoholic beverages have calories but are low in nutritional value. Generally, anything more than moderate drinking can be harmful to your health. Some people, or people in certain situations, shouldn't drink at all. If you have questions or concerns, talk to your doctor.
The Dietary Guidelines for Americans 2005 is available at www.healthierus.gov/dietaryguidelines.





Attention Physicians
Congestive Heart Failure in New York's
Medicaid Population
Drug Therapy Shows Success!
Return to Table of Contents

Congestive Heart Failure (CHF) is a frequent cause of hospitalization, morbidity and mortality in Medicaid patients, accounting for more than 35,000 admissions in 2003*.
Common drug therapy for this condition includes:
- angiotensin converting enzyme inhibitors (ACEI),
- angiotensin receptor blockers (ARB), and
- the beta blockers, carvedilol, metoprolol and bisoprolol,
These drugs have been demonstrated to reduce hospitalization and mortality in CHF patients while improving their quality of life.
A recent New York State Drug Utilization Review study shows that among 17,578 eligible Medicaid recipients discharged from inpatient admissions with a primary or secondary diagnosis of CHF:
- 55% received an ACEI or ARB within 30-days of discharge.
- 41% received a beta blocker in the same time frame.
- 19% received both therapies.
The study also showed that compliance with therapy six-months after discharge appeared excellent, with a large percentage of original recipients receiving ACEI or ARB, beta blockers or both therapies. It has been reported in the literature that 80-90% of CHF patients can tolerate these medications and additional Medicaid patients may benefit from these therapies.
From 2000 to 2003, the use of ACEI or ARB has increased slightly, but the use of beta blockers and both therapies has increased by about 60%.
Providers are encouraged to review the published guidelines for use in their practice.
The American College of Cardiology has published their treatment guidelines on-line at:
http://www.acc.org/clinical/guidelines/failure/hf_index.htm
The American Heart Association has an extensive resource for patients on-line at:
www.americanheart.org/presenter.jhtml?identifier=1486.
* Information taken from the New York State Office of Medicaid Management Data Warehouse.
Graphs displaying the dispensing frequencies of ACEI or ARB and beta blockers for the counties with the greatest number of cases of CHF are provided below:
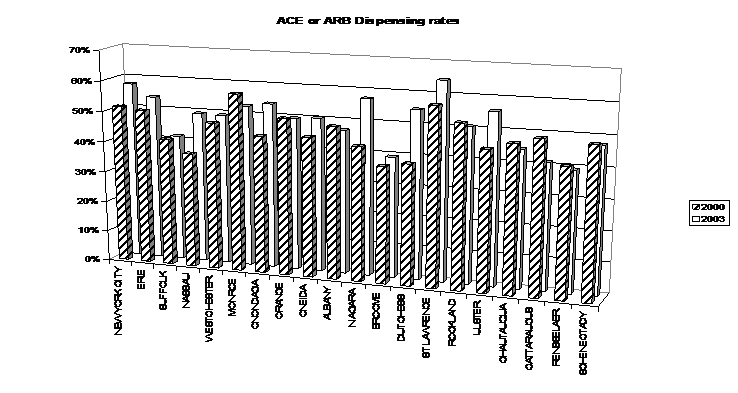
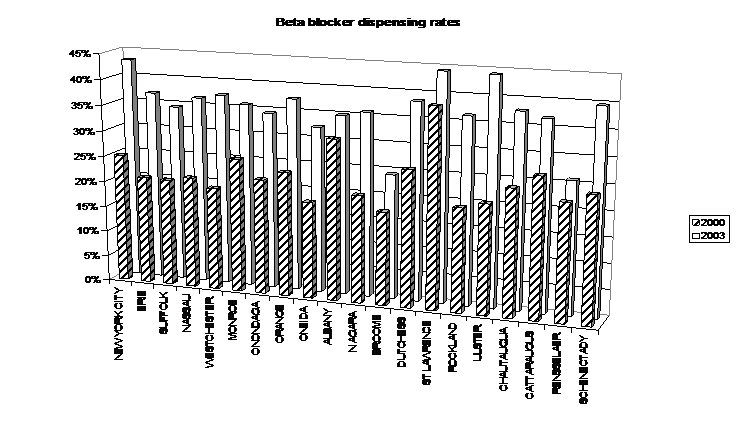
Graphs courtesy of the NYS Department of Health Office of Medicaid Management Data Warehouse
Attention Providers of
Personal Care Services
Consumer Directed Personal Assistance Programs
Personal Emergency Response Services
Assisted Living Programs
Limited Licensed Home Care Service
Prior Authorization Rosters
Available Electronically
Return to Table of Contents
In the December 2004 Medicaid Update , an article introduced the availability of the eMedNY eXchange. Additionally, the CSC website and provider correspondence, have discussed the eMedNY eXchange option.
It is advantageous for you to enroll in eMedNY eXchange, which is accessible through the eMedNY website at www.emedny.org
Although PA rosters for prior authorized long term care services will continue to be printed and mailed to you, enrollment in eMedNY eXchange will allow you to view, print and download your PA rosters weekly.
This will eliminate the delays associated with postal mailing and allow a long term care provider immediate access to their rosters. You will also have the option of downloading your rosters to a personal computer to assist you with your billing process.
Presently, somedistricts mail providers copies of the DSS 2932 (Prior Authorization form) indicating the PA number, client and hours of authorization, however, districts will no longer be required to complete the DSS 2932 form since the HIPAA compliant PA number will be generated by eMedNY.
We urge you to consider enrolling in eMedNY eXchange. You may do so by contacting Provider Services at (800) 343-9000 or via the internet at www.emedny.org.
When you enroll, you must indicate that you want an electronic version of your roster sent to your mail box.
Would You Like Future Medicaid Updates Emailed To You?
Return to Table of Contents
You will receive the Update about 3 weeks before the mailed copy!
Email your request, along with your provider identification number (found on the mailing address label of the update) to: MedicaidUpdate@health.state.ny.us.
Let us know if you want to continue receiving the hard copy in the mail, in addition to the emailed copy.
Reprint from
February 2005
Medicaid Update
Managed Care Enrollee
Pharmacy Co-Payment Changes
PHARMACIES
and
MEDICAID MANAGED CARE PLANS
Return to Table of Contents

As a result of recent changes in State Law, enrollees in Medicaid managed care plans are subject to Medicaid co-payments for pharmacy items.
Beginning April 1, 2005, enrollees in Medicaid managed care plans will have pharmacy co-payments as described below:

| ITEM | CO-PAYMENT AMOUNT | DETAILS ABOUT CO-PAYMENT |
| Brand-Name Prescription Drugs | $2.00 | One co-payment charge for each new prescription
and for each refill NO CO-PAY FOR: Drugs to treat mental illness (psychotropic), tuberculosis, and birth control. |
| Generic Prescription Drugs | $0.50 | One co-payment charge for each new prescription and for each refill
NO CO-PAY FOR: Drugs to treat mental illness (psychotropic), tuberculosis, and birth control. |
| Over-the-Counter Medications | $0.50 | One co-payment charge for each item ordered by a recognized practitioner NO CO-PAY FOR: Birth control items. |
Consistent with fee-for-service Medicaid, the annual co-payment maximum per recipient per year is $100. The benefit year begins April 1 and ends on March 31 of the following year. Once the maximum has been reached, no co-payments will be required until the new benefit year begins.
CO-PAYMENT EXEMPTIONS
The same co-payment exemptions that apply to Medicaid fee-for-service recipients also apply to Medicaid managed care enrollees.
Medicaid managed care enrollees who cannot afford to pay and tell the pharmacist that they are unable to pay must be provided with the ordered pharmacy items. The pharmacy cannot refuse to provide pharmacy items because of a recipient's inability to pay. (Recipients still owe the unpaid co-pay amounts to the pharmacy and may be asked to pay or may be billed.)
Co-payment exemptions include:
- Recipients younger than 21 years old.
- Recipients who are pregnant.
Pregnant women during pregnancy and for the two months after the month in which the pregnancy ends. - Family planning (birth control) services. This includes family planning drugs or supplies like birth control pills and condoms.
- Residents of an Adult Care Facility licensed by the New York State Department of Health (DOH).
- Residents of a Nursing Home.
- Residents of an Intermediate Care Facility for the Developmentally Disabled (ICF/DD).
- Residents of an Office of Mental Health (OMH) or Office of Mental Retardation and Developmental Disabilities (OMRDD) certified residences.
- Enrollees in a Comprehensive Medicaid Case Management (CMCM) or Service Coordination Program.
- Enrollees in an OMH or OMRDD Home and Community Based Services (HCBS) Waiver Program.
- Enrollees in a DOH HCBS Waiver Program for Persons with Traumatic Brain Injury (TBI).
NOTE: Recipients who are eligible for both Medicare and Medicaid and/or receive Supplemental Security Income (SSI) payments are not exempt from Medicaid co-payments, unless they also fall into one of the groups listed above.
Questions regarding the New York State Medicaid Recipient Co-Payment Program should be directed to the Medicaid Helpline at (800) 541-2831.
Your Provider Manual Is Going Online!
Return to Table of Contents

The Department is beginning to make provider manuals available on the internet at:
http://www.emedny.org/providermanuals/index.html
Up to this time, the Medicaid program has relied on a paper provider manual.
- Upon enrollment, the new provider would receive a plastic binder containing policy and billing information.
- When a change was made to the manual, replacement pages would be mailed to the affected provider group(s).
Now, the Department is making an effort to update all manuals and migrate the material to the eMedNY website! New providers will no longer receive the binder of material, nor will changes to existing manuals be mailed to providers. Rather, all necessary information will be available online.
Manuals can be printed, and downloaded to your own computer!
INDEX OF 2004 MEDICAID UPDATE ARTICLES
Return to Table of Contents
Provider/Subject Title of Article Month
All Providers
- Automatic Refills January
- Gifts, Inducements & Remuneration January
- New Types of Common Benefit Identification Cards to be Issued January
- Fee-For-Service Providers January
- Prescribers and Pharmacists: Cialis February
- Diagnosis of Occupational Diseases February
- Enteral Products Classification List February
- Providers Are You Changing Your Correspondence Address or Pay to Address? February
- Provider Audit Protocols March
- Providers of Group Practices - Requirements and Responsibilities in the Medicaid Program March
- Common Physician Practice: Locum Tenens Arrangements/What Does the Agreement Allow? March
- Prescribers and Pharmacy Providers: Medicaid Prescription Requirements Reminder March
- Medicaid Posters and Brochures April
- Prescription Requirements for Carve Out/Pass-Through Drugs May
- Payment of Medicare Coinsurance May
- Group Practice Reminders to Physicians, Dentists and Other Practitioners June
- Medicaid Payments to Physicians for Rapid HIV Testing June
- Medicaid Payment for Psychiatric Social Work June
- New York City Providers: Voluntary Medicaid Managed Care for SSI and SSI-Related Beneficiaries June
- Licensed Home Care Services Agencies and Independent Providers of Private Duty Nursing Services June
- Admission to Rehabilitation Services - Recipient Restriction Program July
- Hospital Responsibility for Outside Care: Reimbursement Policy August
- Medicaid Policy for Erectile Dysfunction Drugs August
- Prescribers of Erectile Dysfunction Drugs: Use Professional Judgment August
- New Laboratory Service Available: Blood Draws in Recipients' Homes September
- Service Provider Number Should Not be the Same as Billing Provider Number September
- Mental Health and Chemical Dependence Providers: SSI Medicaid Managed Care Benefit Package September
- Expanded Syringe Access Demonstration Program (ESAP) September
- Provider Services Fax-on-Demand System Now Available October
- Changes in Prior Approval Codes: Physician and Ophthalmic Providers October
- Medicare, Medicaid and Elderly Pharmaceuticals Insurance Coverage Program October
- Medicaid Purchases: Medicaid Part A Coverage October
- Changes Affecting Prior Approvals/Prior Authorizations November
- How Do I Request Sterilization and Hysterectomy Consent Forms November
- Change in Graphics of the Common Benefit Identification Card December
- Influenza December
- Provider Manuals Online December
Asthma
- Asthma Triggers January
- Medicaid Posters and Brochures April
- The Main Types of Asthma Medications May
- Medicaid Guidelines for the Administration of Xolair July
Billing
- Synagis Procedure Code Correction for Physician Billing January
- Notice to New York State Hospitals Billing DRGs February
- Revised Pharmacy Billing Procedure for Compounded Prescriptions February
- DME and Pharmacy: Fee Schedule Provisions February
- Preferred Physicians and Children's Program Billing Guidelines March
- Clinics: Proper Billing Requirements April
- Notice to Hospitals Billing DRGs April
- Payment of Medicare Coinsurance May
- Physician Billing for Drugs May
- Medicaid Payments to Physician for Rapid HIV Testing June
- Medicaid Payment for Psychiatric Social Work June
- Update to Products of Ambulatory Care/Products of Ambulatory Surgery Groups July
- Ambulette Transportation Providers: Additional Information Required for Billing July
- National Drug Code: Billing Announcement August
- Hospital Responsibility for Outside Care: Reimbursement Policy August
- Orders and Providers of Apnea Monitors August
- Pharmacy Reimbursement Changes September
- New Laboratory Service Available: Blood Draws in Recipients' Homes September
- Physician, Nurse Practitioner, Ordered Ambulatory Billing: New Drug Codes Effective Nov. 1, 2004, October
- Quantity Changes for Infusion Supplies October
- Medicare, Medicaid and Elderly Pharmaceuticals Insurance Coverage Program October
- Inpatient Services Paid "Off-Line" October
- Magnetic Media November
- Ambulette Transportation Providers: Additional Information Required for Billing November
- Reimbursement for Physician-Administered Drugs November
- Physician Assistants November
- Remittance Advices: eMedNy Transaction 820 and 835 December
- Pharmacy Provider: You Must Bill Medicare First December
- NCPDP 5.1 Billing Requirements for Medicare Crossover Claims December
Claims
- Timely Submission of Claims to Medicaid February
- Timely Submission of Claims to Medicaid May
- Service Provider Number Should Not be the Same as Billing Provider Number September
- Non-Emergency Transportation: Electronic Claims and Procedure Codes October
- Dental Claims HIPAA 837D Transaction Change in Oral Cavity Reporting November
- Denial Reports Created December
- Non-Emergency Transportation: Electronic Claims Submission December
- Paper Claim Forms December
Clinic
Clinic Social Worker
Dental
- Requirements and Expectations of Dental Clinics March
- Dental Services Procedures September
- Prior Approval of Orthodontic Services to Spread to Counties Outside of NYC, Nassau and Suffolk September
- Dental Claims HIPAA 837D Transaction Change in Oral Cavity Reporting November
- Do You have a Dental Mobile Van? December
Diabetes
- Diabetes Prevention February
- Be Smart About Your Heart: Control the ABC's of Diabetes April
- Medicaid Posters and Brochures April
- Take Time to Care About Diabetes August
Disease Management
- Diagnosis of Occupational Diseases February
- Pesticide Poisioning Registry April
- A Message from the American Lung Association City of NY June
- Medicaid Payment to Physicians for Rapid HIV Testing June
- NYS Medicaid Smoking Cessation Policy August
- Office of Women's Health Campaign August
- Take Time to Care About Diabetes August
- Arthritis and Exercise September
- The Great American Smokeout November
Drug Coverage
- Prescribers and Pharmacists: Cialis Information February
- Coverage of Plan B by Medicaid June
- Medicaid Guidelines for the Administration of Xolair July
- Medicaid Policy for Erectile Dysfunction Drugs August
- Prilosec OTC Coverage September
- Mandatory Generic Drug Program Update September
- Physician, Nurse Practitioner, Ordered Ambulatory Billing: New Drug Codes October
- Effective November 1, 2004 Quantity Changes for Infusion Supplies October
- Reimbursement for Physician-Administered Drugs November
- Medicaid Coverage for Wireless Capsule Endoscopy November
- Medicaid Coverage of Palivizumab (Synagis) November
Durable Medical Equipment (DME)
- Enteral Formula Prior Authorization February
- Enteral Products Classification List February
- DME and Pharmacy: Fee Schedule Provisions March
- Important Pharmacy and DME Contact Numbers July
- Orders and Providers of Apnea Monitors August
- Changes in Durable Medical Equipment Prior Approval, Rental and Pricing October
- Durable Medical Equipment: Prior Approval Requests November
Educational Tools
- Asthma Triggers January
- How Your Doctor Diagnosis Asthma February
- Tips to Eating Smart March
- The Burden of Arthritis in NY April
- The Main Types of Asthma Medications May
- How to Read Nutritional Labels September
- Dietary Fats and Your Health October
- How Can I Reduce Unhealthy Fat From My Diet November
- Eating Fruits and Vegetables Help Reduce Your Risk of Disease December
- The Role of Proteins in Your Body December
Eligibility
- Pharmacists-New Nursing Home Eligibility Edits and Messaging February
- Medicaid Eligibility Field Software Soon to be Terminated June
- Consult Your Medicaid Eligibility Verification System Manual When Reading Your Printouts June
eMedNY
- eMedNY Phase II Implementation Getting Closer June
- Companion Guides for eMedny Start Up August
- eMedNY Update August
- Draft Companion Guides for eMedNY Start Up September
- Key Changes Under eMedNY Phase II September
- Phase II Will Not Support Blocked Data October
- Phase II Will Continue to Support the "Tilde" October
- Remittance Advices: HIPAA Transaction 835 and 820 October
- Introducing the eMedNY Exchange October
- Non-Emergency Transportation: Electronic Claims and Procedure Codes October
- Changes Affecting Prior Approvals/Prior Authorizations November
- Magnetic Media November
- Remittance Advices: HIPAA Transaction 835 and 820 December
- eMedNY eXchange is Available December
- Encounter Data Submission December
Enrollment
- Fee-For-Service Providers January
- Managed Care Special Needs Plans Expansion of Service Areas January
- Part-Time Clinics Can Learn from Past Actions March
- Providers of Group Practices-Requirements and Responsibilities in the Medicaid Program March
- Pharmacy Providers: Are You Enrolled in Medicaid Yet? May
- Submittal of Current Pharmacy License October
- Medicare Requirement for Pharmacy Enrollment in the Medicaid Program December
ePaces
- ePACES User System Requirements for Optimal Performance March
- Medicaid Eligibility Field Software Soon to be Terminated June
- HIPAA Notes for Medicaid July
Family Health Plus
Family Planning
- Services Available Under the Family Planning Benefit Program June
- Coverage of Plan B by Medicaid June
Fraud
HIPAA
- Urgent Medicaid HIPAA Update May
- Vital Medicaid HIPAA Update June
- Medicaid Eligibility Field Software Soon to be Terminated June
- Urgent Medicaid HIPAA Update: Final HIPAA Deadline Date Set July
- HIPAA Notes for Medicaid July
- HIPAA Deadline Date August
- HIPAA Compliance Deadline: October 6, 2004 September
- Provider Services Fax-on-Demand System Now Available October
- HIPAA Companion Guides for eMedNY Phase II November
- Deadline for End of HIPAA Exception Processing November
- HIPAA Compliance Deadline: December 29, 2004 December
- Denial Reports Created December
Home Health Care
- Licensed Home Care Services Agencies and Independent Providers of Private Duty Nursing Services June
- New Laboratory Service Available: Blood Draws in Recipients' Homes September
Hospital
Managed Care
- Managed Care Special Needs Plans Expansion of Service Areas February
- NYC Providers: Voluntary Medicaid Managed Care for SSI and SSI-Related Beneficiaries June
- Expansion of Service Areas: Managed Care Special Needs Plan August
- Mental Health and Chemical Dependence Providers: SSI Medicaid Managed Care Benefit Package September
- Expansion of Managed Care: Special Needs Plans Service Areas October
MEVS
- Consult Your Medicaid Eligibility Verification System Manual When Reading Your Printouts June
- New Coverage Codes Announced July
- New Coverage Codes Reminder: Resource Attestation to be Implemented August
Nursing Home
Pharmacy
- Automatic Refills Number January
- Pharmacists-New Nursing Home Eligibility Edits and Messaging February
- Revised Pharmacy Billing Procedure for Compounded Prescriptions February
- DME and Pharmacy: Fee Schedule Provisions March
- Pharmacy Providers: Are You Enrolled in Medicaid Yet? May
- Important Pharmacy and DME Contact Numbers July
- Pharmacy and Reimbursement Changes September
- Submittal of Current Pharmacy License October
- Ask The Pharmacist October
- Pharmacy Providers: You Must Bill Medicare First December
Physician
- Synagis Procedure Code Correction for Physician Billing January
- Common Physician Practice: Locum Tenens Arrangements/What Does the Agreement Allow? March
- Physician Billing for Drugs May
- Group Practice Reminders to Physicians, Dentists and Other Practitioners June
- Reimbursement for Physician-Administered Drugs November
- Physician Assistants November
Prior Authorization
- Enteral Formula Prior Authorization February
- Prior Authorization Tips for Prescribers May
- Second Generation Antihistamine Prior Authorization Reminder October
- Changes Affecting Prior Approvals/Prior Authorizations November
Products of Ambulatory Care (PAC)
Restriction
- Referral Process: Recipient Restriction Program July
- Admission to Rehabilitation Services-Recipient Restriction Program July
Residential Facilities
Transportation
- Update to Products of Ambulatory Care/Products of Ambulatory Surgery Grouper July
- Ambulette Transportation Providers: Additional Information Required for Billing July
- Hospital Responsibility for Outside Care: Reimbursement Policy August
- Transportation Providers and Subcontracting Transports August
- Non-Emergency Transportation: Electronic Claims and Procedure Codes October
- Ambulette Transportation Providers: Additional Information Required for Billing November
- Do You Have a Dental Mobile Van? December
Utilization Threshold
Vision Care
The Medicaid Update: Your Window Into The Medicaid Program
The State Department of Health welcomes your comments or suggestions regarding the Medicaid Update.
Please send suggestions to the editor, Timothy Perry-Coon:
NYS Department of Health
Office of Medicaid Management
Bureau of Program Guidance
99 Washington Ave., Suite 720
Albany, NY 12210
(e-mail MedicaidUpdate@health.state.ny.us)
The Medicaid Update, along with past issues of the Medicaid Update, can be accessed online at the New York State Department of Health web site: http://www.health.state.ny.us/health_care/medicaid/program/main.htm